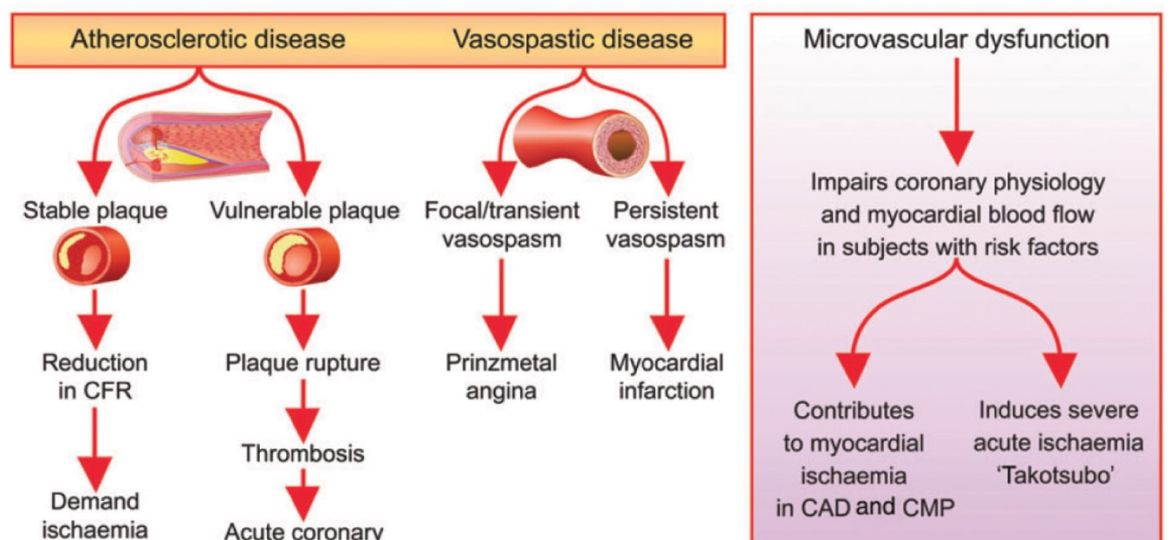
How important is microcirculation in clinical practice?
This study explores the microcirculation in patients with acute heart failure (AHF) and cardiogenic shock (CS). It highlights the importance of evaluating microcirculatory function alongside traditional hemodynamic measures in these patients.

Microcirculatory dysfunction, characterized by impaired blood flow at the capillary level, is linked to poorer outcomes in AHF and CS. The study suggests that interventions targeting microcirculation could potentially enhance patient outcomes in these conditions. In summary, understanding and addressing microcirculatory dysfunction is crucial for managing AHF and CS effectively.
Read the full study: https://academic.oup.com/eurheartjsupp/article/21/Supplement_B/B25/5422922
Acute heart failure (AHF) and its treatment
Acute heart failure (AHF) is a condition characterized by a sudden onset or worsening of symptoms related to the heart’s inability to pump blood effectively. This can lead to a buildup of fluid in the lungs and other tissues, causing symptoms such as shortness of breath, fatigue, and swelling in the legs and ankles. AHF can be caused by various factors, including heart attack, infections, arrhythmias, high blood pressure, or underlying heart conditions.
The diagnosis of AHF is based on a combination of clinical symptoms, physical examination, and diagnostic tests such as echocardiography and blood tests. Treatment aims to alleviate symptoms, improve heart function, and address the underlying cause. It may include medications such as diuretics to remove excess fluid, vasodilators to relax blood vessels, inotropic agents to strengthen heart contractions, and oxygen therapy to improve oxygenation.
In severe cases, AHF can lead to cardiogenic shock, a life-threatening condition where the heart’s pumping function is severely compromised, necessitating urgent medical intervention. Long-term management of AHF often involves lifestyle modifications, medication adherence, and regular follow-up with healthcare providers to prevent future episodes and complications.